|
Refer for displaced or unstable fractures Increase flexion by 15 degrees weekly, from 45 degrees to full extensionĮxtensor tendon avulsion from the base of the distal phalanxĬontinuous extension in the splint for six to eight weeks is essentialĪcute carpal bone fractures (excluding scaphoid/trapezium)Ĭhildhood buckle fractures of the distal radiusĬonsider splinting as definitive treatment for buckle fractures Middle phalangeal volar plate avulsions and stable reduced PIP joint dislocations Refer for angulated, displaced, rotated, oblique, or significant intra-articular fracture or failure to regain full range of motionĮncourage active range of motion at PIP and MCP joints Nondisplaced proximal/middle phalangeal shaft fracture and sprainsĮncourage active range of motion in all joints Refer for angulated, displaced, intra-articular, incompletely reduced, or unstable fracture Stable thumb fractures with or without closed reductionįracture of the middle/proximal one third of the scaphoid treated with casting Nondisplaced, nonangulated, extra-articular first metacarpal fractures Thumb, first metacarpal, and carpal bones Second and third proximal/middle phalangeal shaft fractures and select metacarpal fractures Refer for angulated, displaced, rotated, oblique, or intra-articular fracture or failed closed reduction Proper positioning of MCP joints at 70 to 90 degrees of flexion, PIP and DIP joints at 5 to 10 degrees of flexion This article highlights the different types of splints and casts that are used in various circumstances and how each is applied.įourth and fifth proximal/middle phalangeal shaft fractures and select metacarpal fractures Indications and accurate application techniques vary for each type of splint and cast commonly encountered in a primary care setting. Selection of a specific cast or splint varies based on the area of the body being treated, and on the acuity and stability of the injury. All patients who are placed in a splint or cast require careful monitoring to ensure proper recovery. 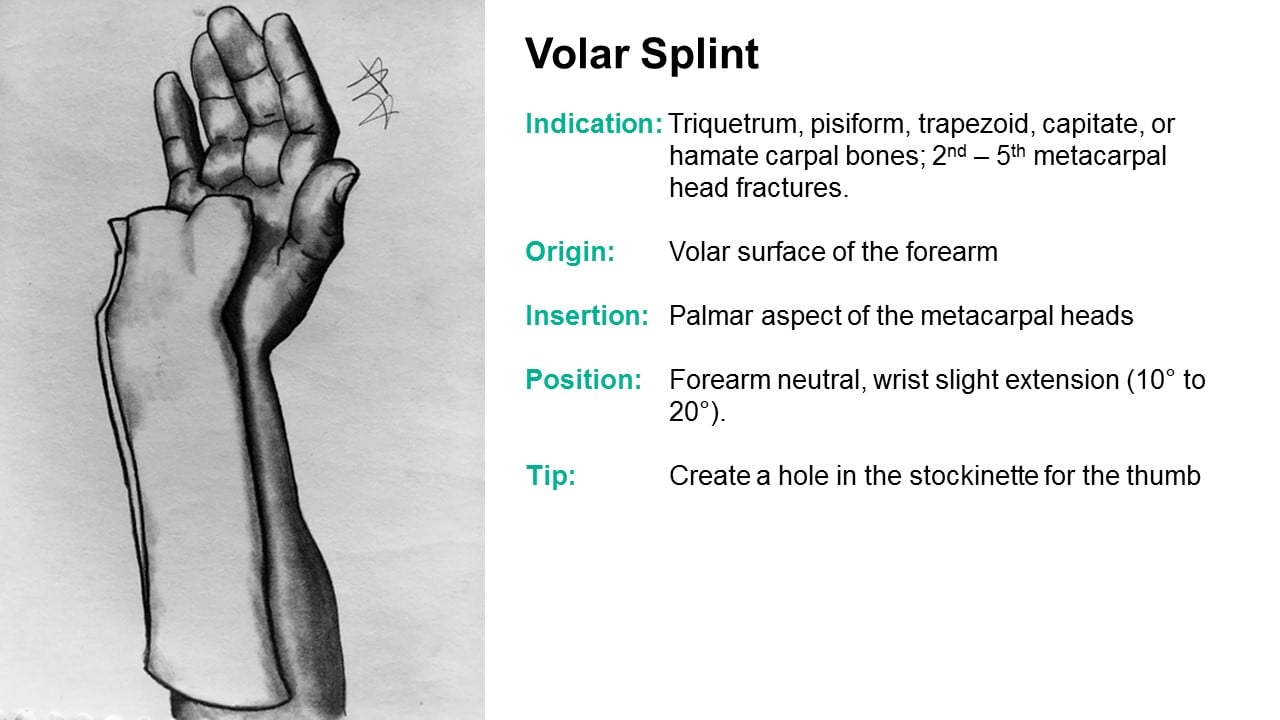
Excessive immobilization from continuous use of a cast or splint can lead to chronic pain, joint stiffness, muscle atrophy, or more severe complications (e.g., complex regional pain syndrome). To maximize benefits while minimizing complications, the use of casts and splints is generally limited to the short term. Because of this, casts provide superior immobilization but are less forgiving, have higher complication rates, and are generally reserved for complex and/or definitive fracture management. This quality makes splints ideal for the management of a variety of acute musculoskeletal conditions in which swelling is anticipated, such as acute fractures or sprains, or for initial stabilization of reduced, displaced, or unstable fractures before orthopedic intervention. Splints are noncircumferential immobilizers that accommodate swelling. Treatment of radial head fractures depends on the specific characteristics of the fracture using the Mason classification.Management of a wide variety of musculoskeletal conditions requires the use of a cast or splint. Radial head fractures may be difficult to visualize on initial imaging but should be suspected when there are limitations of elbow extension and supination following trauma. Combined fractures involving both the ulna and radius generally require surgical correction. These fractures are treated with immobilization or surgery, depending on the degree of displacement and angulation. Isolated midshaft ulna (nightstick) fractures are often caused by a direct blow to the forearm. 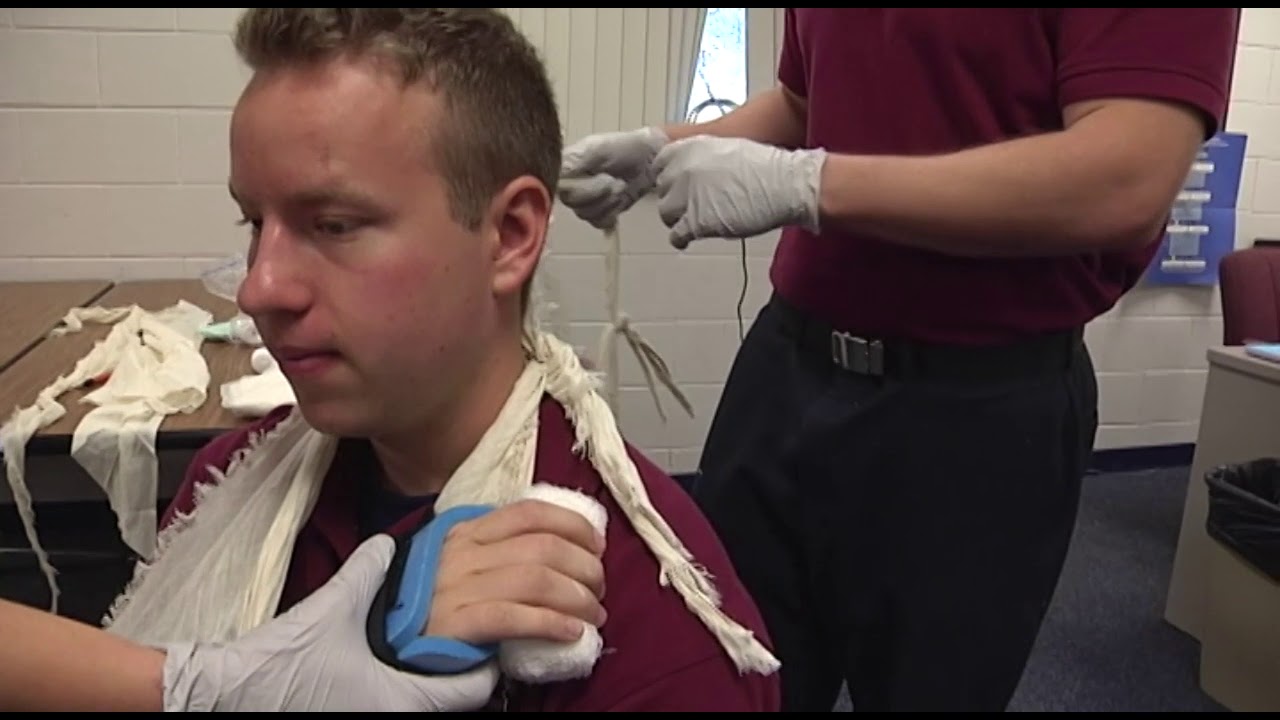
It should be noted that these fractures may be complicated by a median nerve injury. A nondisplaced, or minimally displaced, distal radius fracture is initially treated with a sugar-tong splint, followed by a short-arm cast for a minimum of three weeks. In adults, distal radius fractures are the most common forearm fractures and are typically caused by a fall onto an outstretched hand. Depending on the degree of angulation, buckle and greenstick fractures can be managed with immobilization. Greenstick fractures, which have cortical disruption, are also common in children. Incomplete compression fractures without cortical disruption, called buckle (torus) fractures, are common in children. If initial imaging findings are negative and suspicion of fracture remains, splinting and repeat radiography in seven to 14 days should be performed. Evaluation with radiography or ultrasonography usually can confirm the diagnosis.  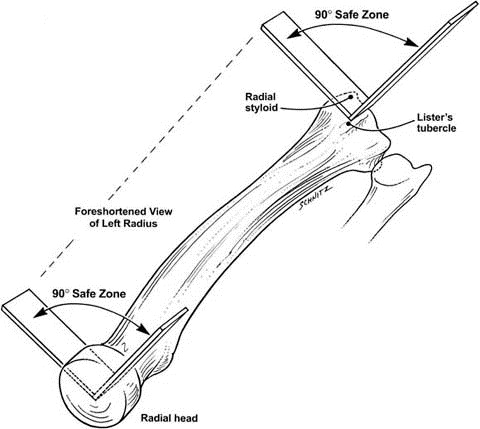
A fall onto an outstretched hand is the most common mechanism of injury for fractures of the radius and ulna. Fractures of the radius and ulna are the most common fractures of the upper extremity, with distal fractures occurring more often than proximal fractures.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
